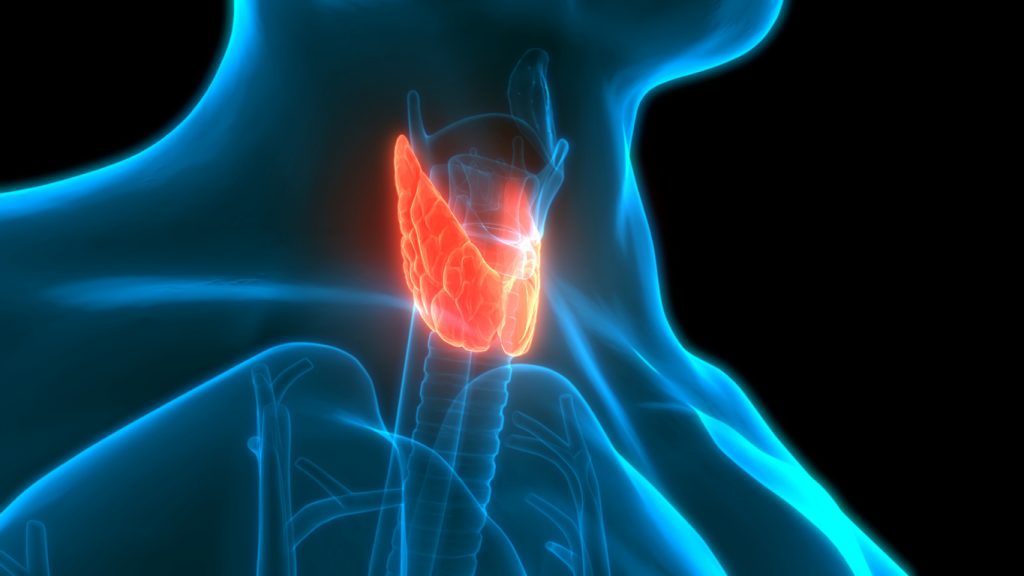
The thyroid is a butterfly shaped gland that sits just below and behind the larynx (Adam’s apple) and in front of the trachea (windpipe). Thyroid hormone regulates the metabolic rate – – the sum of cellular processes that create cellular energy. If you were a car, your rate of metabolism could be described as the gear you are in.
Imbalances in thyroid function can result from either deficient or excessive hormone production. The pituitary gland produces thyroid-stimulating hormone (TSH) that directs the thyroid gland to make more thyroid hormone.
Deficiency of thyroid hormone is called hypothyroidism and can range from mild to severe. Inasmuch as thyroid hormone affects every organ, tissue, and cell in the body, disturbances in thyroid function results in many and varied symptoms. An excess of thyroid hormone is called Graves Disease, or hyperthyroidism. It is less common than hypothyroidism.
This discussion of thyroid disease is restricted to hypothyroidism, a much more common disease than hyperthyroidism.
Signs and Symptoms of Thyroid Hormone Deficiency
- Low body temperature
- Tiredness and fatigue
- Slow to waken in the morning
- Weight gain and difficulty losing weight
- Depressed mood
- Poor mental function
- Constipation
- Cold hands and feet
- Obesity
- Dry skin
- Orange discoloration of palms and soles
- Goiter
- Thinning or disappearance of outer eyebrows
- Edema (swelling) of face, tongue, ankles, and fingersDry, brittle hair
- Migraines
- Hair loss
- Fibrocystic breasts
- Altered menstrual periods and ovarian cysts
Signs and Symptoms of Thyroid Hormone Excess
- Anxiety
- Tremulousness
- Difficulty sleeping
- Difficulty gaining weight
- Voracious appetite
- Heart palpitation and bounding, rapid heart rate
- Moist skin
- Frequent bowel movements
- Heat intolerance
- Muscle cramps
- Jittery feeling
- Hyperventilation
- Facial expression of anxiety
- Eyes appear wide open or startled (exophthalmus)
Because many of the symptoms of low thyroid hormone levels are of a general nature (fatigue, obesity, constipation, dry skin), the diagnosis can be overlooked, often for years. If a person is deficient in thyroid hormone, the symptoms of deficiency will not respond satisfactorily to anything but the replacement of what is missing. Thyroid replacement therapy is usually given long term.
Subclinical Hypothyroidism
Subclinical hypothyroidism is a condition that occurs when many of the above signs and symptoms of deficient thyroid hormone are present, but laboratory measurements of thyroid hormone commonly performed at doctors’ offices, are within the normal range. Some patients with hypothyroidism have been wrongly labeled as having psychosomatic illness because their blood tests appear normal. Special thyroid laboratory blood tests will often, however, detect thyroid deficiencies in these individuals.
Years ago, before blood tests and synthetic drugs were available, doctors relied on patients’ histories and physical exams to diagnose and treat them. If patients presented with symptoms and physical findings that fit the clinical picture of hypothyroidism, they would then be prescribed the only agent available at that time, whole glandular thyroid from pig thyroid. This preparation, still available as a prescription drug, is known as Armour Thyroid, contains mostly T4 (a mostly inactive form of thyroid hormone that needs to be converted to T3 in the body) and, in addition, T3 (the biologically active form of thyroid hormone).
A small but growing group of doctors have continued this tradition of listening to patients’ symptoms and performing a careful physical examination in addition to using blood tests. They have continued to treat hypothyroidism with natural, whole, desiccated thyroid gland. This natural time-tested approach more often results in improvement in mood and mental functioning-symptoms often not improved by the more commonly used prescription drugs.
A low basal body temperature raises suspicion of subclinical hypothyroidism. A basal body temperature is determined by taking the temperature in the armpit for ten minutes the very first thing in the morning before getting out of bed, using an “old fashioned” mercury thermometer that has been shaken down the night before. Do this for four or five consecutive mornings and record the results. A temperature consistently below 97.6 is suggestive of hypothyroidism.
Laboratory Testing
In Hypothyroidism: The Unsuspected Illness, Broda Barnes, M.D., states: “It may seem incredible that scientists can sit quietly on earth and follow the activity of the heart of a man walking on the moon and yet they have had so much difficulty in measuring the amount of thyroid hormone necessary for health and in developing effective and reliable tests to determine when thyroid function is inadequate.”
Many laboratory tests for measuring thyroid hormone have come and gone since Dr. Barnes made that statement in 1976. The fact remains that the road one travels while treating hypothyroidism based on laboratory tests can be strewn with potholes. Every doctor who treats hypothyroidism has seen discrepancies when comparing blood test results with how patients report feeling.
There has been a reliance among doctors on measuring TSH levels to ascertain what the pituitary is telling the thyroid to do, knowing that a high TSH results when the pituitary tries to stimulate a low functioning thyroid gland. True enough.
However, a low TSH is not as specific. It could mean that there is excessive thyroid hormone resulting in the pituitary stopping the stimulation of more thyroid hormone. Or it could be low as a result of a person being appropriately treated with thyroid hormone, as the pituitary senses that it need not stimulate the thyroid to make more hormone.
Some physicians are concerned with a low TSH level in a patient on supplemental hormone, believing that it is evidence that there is interference with a sophisticated finely tuned feedback system that naturally regulates thyroid hormone production. The mere fact that a person requires hormone replacement implies that the feedback system, regardless of its sophistication, has failed to create homeostasis, or balance. Careful prescribing of thyroid replacement hormone through monitoring of specific laboratory tests can remove the burden of making hormone on an already exhausted thyroid gland, and do not rely solely on TSH levels to determine dosing of thyroid hormone.
Treatments to Address Hypothyroidism
Thyroid hormone replacement therapy requires a doctor’s prescription. And for good reason. A person on the wrong dose of thyroid hormone can feel terrible and have anxiety-producing, even life-threatening, symptoms. Periodic physical exams and monitoring of blood levels of thyroid hormone must be continued on a regular basis.
Two people taking the same dose of thyroid hormone can have greatly differing responses. In fact, the same person taking the same dose of thyroid hormone for years can suddenly react very differently to that same dose with the changes of aging, stress, or the addition of other hormones to his therapy. And a person may episodically need a different replacement dose of thyroid during times of increased stress.
Most physicians who treat hypothyroidism do so with synthetic T4 (Synthroid, Levoxyl, or Unithroid). In the body, T4 has to be converted into triiodothyronine (T3), the biologically active form of the hormone. For several reasons, many people can’t convert T4 to T3, which may result in the symptoms of hypothyroidism. Unfortunately, in this situation, the blood tests that many doctors routinely use to check thyroid status may be normal, which would cause a physician to rule out the diagnosis.
An article in the New England Journal of Medicine reported research suggesting Synthroid use resulted in no improvement in 17 parameters measuring memory, mood, language, and learning. The use of Armour thyroid however, resulted in improvement in 6 of the 17 parameters. (NEJM 1999;340:424-429, 469-470.)